Ask a Periodontist (FAQs)
- If I get treatment now, can I save my teeth?
- Can dental implants develop periodontal disease from my existing teeth with periodontal disease?
- Are dental implants a panacea or should we strive to save teeth?
- How effective is laser treatment for gum disease?
- Do you really need to have all your teeth extracted?
- How does your perio care fare?
- How much will the treatment cost?
General Questions about Periodontics
Why was I referred to a periodontist?
Your general dentist has determined that your gums require special care, and has referred you to a periodontist. Periodontists are dentists who specialize in the diagnosis, treatment and prevention of gum disease. By referring you to a periodontist, your dentist is showing a strong commitment to optimal dental care.
To help you understand why the treatment might be needed, and how your teeth can be saved, Dr. Bleier will attempt to provide answers to some of the most frequently asked questions about periodontal therapy.
What is a periodontist?
Periodontists have had extensive advanced training in the treatment of periodontal disease, a minimum of two years in addition to dental school. As specialists, they devote their time, energy and skill to helping people who need periodontal treatment. Periodontics is one of the eight specialties recognized by the American Dental Association.
What is the relationshipo between general dentist and periodontist?
- Your Dentist
Your dentist and periodontist work together as a team to provide you with the best possible care. They will combine their experience to formulate the best treatment plan for you while keeping each other informed about your progress. - The Periodontist
After active periodontal treatment is completed, the periodontist will refer you back to your general dentist, but may also see you periodically for follow-up care and periodontal treatment. - Self Referrals
Dr. Bleier frequently sees new patients who are self referred. These patients know they have a dental periodontal problem after speaking with physicians, friends and family members. They are savvy from reading health related articles on the connections between periodontal diseases and systemic diseases such as cardiovascular diseases, diabetes, respiratory diseases, cancer, dementia and osteoporosis. Dr. Bleier, at the appropriate time during or after active periodontal treatment and as needed will consult with your physician and will gladly refer you to one of the outstanding general dentists he regularly consults with for the best interests of you, the patient. - The Patient
In closing, remember that the most important member of the team is you. Your interest, participation and commitment are essential to make your treatment a success.
What is periodontal disease?
Periodontal disease is the major cause of about 70 percent of adult tooth loss, affecting three out of four persons at some point in life.
The main cause of gum disease is bacterial plaque, a sticky, colorless film that constantly forms on your teeth. If the plaque is not removed, it hardens into a rough, porous deposit called calculus, or tartar. Toxins (or poisons) produced by the bacteria in plaque irritate the gums and can make them red, tender, swollen and more likely to bleed easily.
As the disease progresses, the toxins destroy supporting tissues around teeth, forming pockets that fill with more plaque. Bone that supports the tteth may be permanently damaged. Unless treated, the affected teeth can become loose and eventually lost.
Conscientious removal of plaque by brushing, flossing and professional cleanings can minimize the risks of gum disease. However, other factors can affect the health of your gums, such as hereditary factors, stress, diabetes and pregnancy.
What are the benefits of periodontal treatment?
Periodontal treatment is an investment in your health. Treating periodontal problems will help you achieve a healthy mouth as well as help you keep a healthy and help prevent tooth loss. In fact, with prompt treatment, proper home care and regular dental visits, the great majority of patients can keep their teeth for a lifetime.
What does periodontal treatment involve?
After reviewing your medical and dental history, the periodontist will examine your gums, teeth and mouth. This examination will include looking at the color and firmness of your gums, studying which teeth are loose and checking how much gum tissue has been lost. Necessary radiographs may be taken to evaluate the bone supporting the teeth.
After gathering this information, the periodontist will discuss your condition with you and suggest the most helpful treatment for your dental health.
In the earlier stages of gum disease, most of the treatment involves scaling and root planing, which means removing plaque and calculus in the pockets around the tooth and smoothing the root surfaces. In most cases of early gum disease, scaling, root planing and proper daily cleaning of the teeth are all that are required for a satisfactory result, others require topical or systemic antimicrobials. Treatment is tooth or site specific with many teeth restored to good periodontal health without the need for the surgical phase of treatment.
More advanced cases may require surgical treatment. The goals of this treatment are to remove calculus from deep pockets around the teeth, shrink the pockets, smooth root surfaces and arrange gum tissue into a shape that will be easier to keep clean. The periodontist is trained to deal with many varieties of gum disease. Whatever your treatment plan entails, the periodontist’s goal is to bring you to a state of good oral health, and then help you maintain it.
Does periodontal treatment hurt?
No. Dr Bleier and his hygiene team have excellent clinical skills that do not require ever using local anesthetics or pain controlling drugs for non-surgical treatments such as scaling and root planning or regular periodontal recall maintenance visits. If teeth are sensitive or painful, he will find out why and treat the cause(s) before beginning periodontal therapy at those specific teeth, to ensure your comfort.
Improved equipment, local anesthetics and modern techniques make periodontal treatment more comfortable now than ever before. Effective medications (although often not necessary) are available to give you comfort after treatment. As with other aspects of periodontal treatment, considerations for your comfort during and after treatment will be tailored to best suit your individual needs.
Dental Health Questions
Is periodontal disease congageous?
Research has shown that periodontal disease is caused by the inflammatory reaction to bacteria under the gums, so periodontal disease technically may not be contagious. However, the bacteria that cause the inflammatory reaction can be spread through saliva. This means that if one of your family members has periodontal disease, it’s a good idea to avoid contact with their saliva by not sharing eating utensils or oral health equipment. If you notice that your spouse or a family member has the warning signs of a possible periodontal problem, (bleeding, red and swollen gums, or bad breath) you may want to suggest that they see the periodontist for an exam; it may help to protect the oral health of everyone in the family.
Is there a link between gum disease, alzheimer’s and dementia?
Gum disease may be linked to Alzheimer’s disease, a small new study suggests. The study was published recently in the Journal of Alzheimer’s Disease. Researchers analyzed brain samples from 10 people with Alzheimer’s and 10 people without the brain disease and found gum disease-related bacteria in the brain samples from four of the 10 Alzheimer’s patients. No such bacteria was found in the brain samples from people without Alzheimer’s.
“This clearly shows that there is an association between oral bacteria and Alzheimer’s disease, but not causal association”, study author Lakahmyya Kesavalu, an associate professor in the College of Dentistry at the University of Florida, said in a university news release. The study is the first to show such a link, the researchers said.
Bacteria in the mouth can enter the bloodstream during chewing, brushing, flossing and dental procedures. The bacteria can travel in the blood to the brain and can potentially lead to brain tissue degeneration that appears similar to Alzheimer’s, the researchers said. Each time the bacteria can enter the brain, the researchers note, this could potentially trigger immune system responses, causing the release of excess chemicals that can kill neurons.
The researchers say that this activity could lead to symptoms such as confusion and deteriorating memory. Previous University of Florida research on mice found that gum disease-related bacteria was able to move from the mouth to the brain.
The study adds to previous findings that Alzheimer’s is linked to poor oral health and oral hygiene. Research from New York University in 2010 revealed long-term evidence that link gum inflammation and Alzheimer’s disease, finding that gum disease could increase the risk of cognitive dysfunction. They add that future research will involve determining whether the Periodontal Pathogen Porphyromones Gingivalis could be used as a marker for a blood test that predicts the development of Alzheimer’s disease in patients who are at higher risk. Diagnostic periodontal and peri-implant microbiology analysis services are available at my office in Endicott, NY.
Can good oral hygiene reduce cancer risk?
A Lancet Oncology Journal study suggests that taking care of your teeth and gums may lower your chances of developing several types of malignancies. The Lancet Oncology study finds that men with a history of periodontal (gum) disease may be at greater risk for several types of cancer. In studying 48,375 men, ages 40-75, researchers found that compared to those without gum disease, men with a history of it had a 14 percent greater risk of cancer, specifically lung, kidney, pancreatic and blood cancers. The increased risk persisted even in men who had never smoked.
The study adds to earlier research suggesting a link between periodontal disease and increased risk for cardiovascular disease and diabetes.
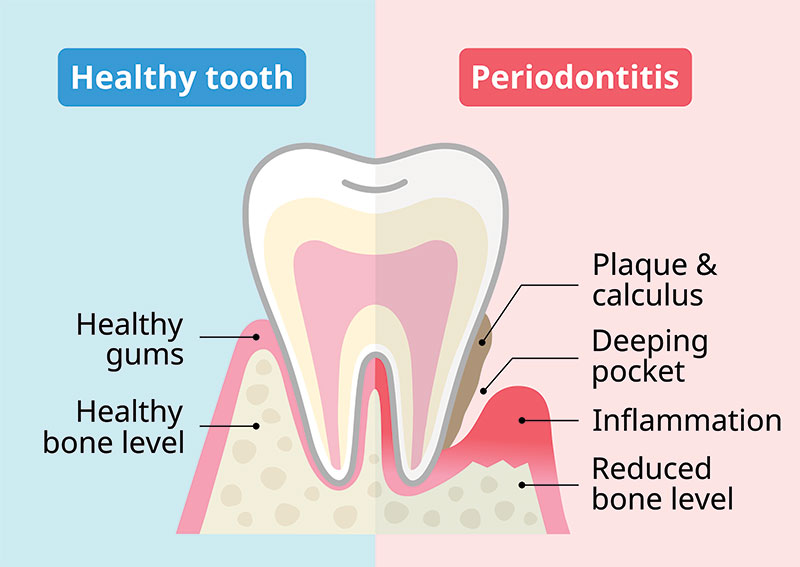
Gum disease occurs when plaque accumulates below the gum line, triggering an immune response that can destroy the tissue and bone that anchor the teeth.
Inflammation to blame?
Evidence suggests that inflammation, the body’s immune response to injury or infection, plays a role in cardiovascular disease and cancer.
Starches and sugars in the food you eat combine with bacteria in your mouth to form plaque, which causes tooth decay. If you don’t clean your teeth, bacteria accumulate beneath your gum line and can trigger an inflammatory response. The body generates inflammation to fight this periodontal infection, but in doing so it can cause more damage. If you let bacteria build up and not be cleaned on a regular basis, the body is going to try to fix things for you.
Inflammation eventually causes pockets between your gums and teeth that fill with bacteria and inflammatory substances. Eventually, the pockets grow deeper and can destroy the connective tissue and bony structures that anchor the teeth, resulting in tooth loss. At this point, the dangerous mix of bacteria and inflammatory substances can then access the bloodstream and travel throughout the body. It is this process that experts believe may link periodontal disease to systemic diseases, such as cancer.
Take care of your teeth and gums
The researchers noted that further studies are needed to confirm whether periodontal disease actually causes cancer and if good oral health can reduce cancer risk. Regardless, you don’t need more reasons to maintain a healthy mouth. Dr. Larry P. Bleier is a Board Certified Harvard Trained Diplomate Periodontist who utilizes the latest techniques in the diagnosis and treatment of gum disease.
There is no substitute for keeping your own natural teeth in health and comfort for a lifetime if you know how. Dr. Bleier can show you how.
Can brushing and flossing correctly add years to my life?
Bacteria, which can find a home and a feast between your teeth and under your gums, can stir up a low-grade gum infection and a simmering inflammatory response that increases your risk of heart disease 72% according to the Cleveland Clinic Chief Wellness Officer, Dr. Michael Roizen, M.D. You will need to brush and floss correctly 60 seconds a day to add an additional 6.4 years to your life according to Dr. Roizen M.D.
Dr. Larry P. Bleier is an expert in the treatment and control of Periodontal/Gum Diseases and can also provide you with the life time skills to correctly floss and brush the teeth and gums for optimal tooth and periodontal gum health.
Is gum disease a significant public health concern?
The Centers for Disease Control and Prevention suggest more American adults may have periodontal disease that “may have been underestimated by as much as 50 percent”. The implication is that more Americans may suffer from moderate to severe gum disease than previously thought making it essential to correct periodontal disease earlier in order to maintain healthy teeth and gums, starting in childhood.
Quoting Dr. Stephen Sinatra, a Cardiologist, in Heart, Health & Nutrition, a Cardiologist’s Guide to Total Wellness, “It’s often been said the eyes are the windows of the soul; I think the mouth is the window of the heart. In fact, I can tell a lot about a patient’s heart health by knowing what type of report they got from their dentist. That’s because there’s a very strong link between gum disease and heart disease risk.”
“This isn’t new. In 1998, the American Academy of Periodontology issued a strong warning that gum infections represent a ‘far more serious threat’ to health of millions of Americans than previously realized. However, it seems people are not giving this important issue the attention it deserves, which is why it stand to be repeated.”
Heart Disease can start in your mouth. Studies have revealed a connection between dental health and cardiovascular health.
Gum disease is an infectious, inflammatory condition caused by bacteria growing on teeth in the form of a dental plaque biofilm. These infections, which can last for decades, put enormous stress on the immune system. Destructive microorganisms, inflammatory compounds, and poisonous waste materials from destroyed bacteria (endotoxins) can all seep from the mouth and circulate throughout the body-creating a systematic hyperimmune and inflammatory situation.
In the bloodstream, research has found periodontal bacterial biofilms invading susceptible arteries and defective heart valves. The bloodstream swarms with antibodies against these common oral microorganisms, but as the disease progresses, the antibodies also attack damaged tissue.
These microorganisms present in gum infections may get into the bloodstream and generate a direct inflammatory stimulus in the body, initiating or contributing to cardiovascular risk. Among the major organisms is Porphyromones gingivalis, a bacterium with a platelet aggregation effect, which means it can cause abnormal clotting.
Another indirect factor may relate to people who have a genetic hyprinflammatory response to infection. They react to localized gum infection by processing excess levels of inflammatory substance in the body-such as C-reactive protein and interleukin-6. High levels of these substances have been identified as risk factors for heart disease because they damage the arteries.
Is tooth loss inevitable as we age?
Maintaining healthy teeth and gums can help you keep your teeth for life
In the late 1500’s, author William Shakespeare and others spoke and wrote about getting long in the tooth as the gums recede as you age. Not so long ago, it was rare for an older person to go to bed without taking out his or her dentures. However, edentulism (toothlessness) has been declining in this country since the 1950s. According to the Centers for Disease Control and Prevention (CDC), approximately 25 percent of the current population over age 65 is toothless.
Periodontal disease is the leading cause of tooth loss in older adults. “However, people should realize that while their likelihood of developing periodontal disease does increase with age, maintaining periodontal health can help you keep your natural teeth for a lifetime”, says Dr. Larry P. Bleier. “Not everyone can avoid the signs of aging, such as wrinkles or the need for bifocals, but periodontal disease can often be prevented.”
A variety of risk factors make older individuals especially susceptible to periodontal disease especially the presence of other diseases. Research has shown a connection between periodontal disease and other inflammatory diseases of aging, such as diabetes, rheumatoid arthritis or heart disease. Other factors that may influence the progression of gum disease include medications, mental health, worsening memory, diminished salivary flow and functional impairments.
“To help prevent periodontal disease and maintain a healthy, toothy smile as you age, it is important to keep your dental professional up to date on any changes in your overall health,” said Dr. Bleier. “The goal is to make adjustments in oral care before these changes result in full-blown problems in the mouth.”
Dr. Bleier recommends comprehensive daily oral care, including regular brushing and flossing, and other hygiene products tailored to your individual needs to avoid gum disease. If gum disease develops, a consultation with a periodontist, can lead to effective treatment based upon sound research and the use of safe well studied techniques. A periodontist is a dentist with three years of additional specialized training in the prevention, diagnosis and treatment of diseases affecting the gums and supporting structures of the teeth and in the placement of dental implants. “An ounce of prevention and early detection is worth a pound of cure.”
Procedure Related Questions
If I get treatment now, can I save my teeth?
Do you have:
- Red, swollen or tender gums
- Receding gums or bad breath
- Loose or shifting teeth from progressive bone loss under the receding gums
- Tooth sensitivity or painful teeth
All the above are warning signs of periodontal disease, a serious infection that if left untreated, can lead to tooth loss. The #1 reason adults lose their teeth.
Periodontal disease causing bacterial pathogens have been implicated in some destructive peri-implant diseases. Catch this bone loss that occurs with periimplantitis as soon as possible! The implant bone loss is not reversible and if not treated can be lead to greater bone loss.
Dr. Larry P. Bleier is a Board Certified Harvard Trained Diplomate Periodontist who utilizes the latest techniques in the diagnosis and treatment of gum disease.
Dr. Bleier has successfully treated thousands of patients with gum problems in over thirty years of practice. His philosophy of treating gum disease is a conservative nonsurgical approach whenever possible.
Dr. Bleier and his staff will help restore your smile and help find solutions to your dental needs. This may involve consulting and working with other dentists as a team to provide you with the best treatment options. There is no substitute for keeping your own natural teeth in health and comfort for a lifetime if you know how. Dr. Bleier can show you how.
Can dental implants develop periodontal disease from my existing teeth with periodontal disease?
Yes, having active untreated periodontal disease is an internationally well known risk factor for the infection spreading to dental implants placed in the same mouth.
Both peri-implant mucositis and peri-implantitis are characterized by an inflammatory reaction in the tissues surrounding a dental implant that can lead to tissue destruction and ultimately, implant failure. Peri-implant mucositis is confined to the soft tissue with no sign of supporting bone loss. Peri-implantitis, similar to periodontitis, results in inflammation around the soft tissue as well as progressive bone loss. Additionally, peri-implant mucositis may be successfully treated using nonsurgical efforts if detected early, whereas periimplantitis usually requires surgical treatment.
Recent reports revealed that peri-implant mucositis was present in 48 percent of implants followed from 9 to 14 years after placement. However, because peri-implant mucositis is reversible with early intervention, it is quite possible that its prevalence could be under-reported. Research concerning peri-implantitis reported distinct differences in the incidence and prevalence from numerous authors with studies ranging from 6.61 percent disease prevalence over a 9-14 year period to 36.6 percent with a mean of 8.4 years after loading.
According to Paul Rosen, DMD, MS, Chair of the AA P Task Force on Peri-implantitis, “Although there are widespread clinical reports where dental implants have achieved long-term success, it is important for dental professionals to understand that peri-implant mucositis or peri-implantitis may arise from a failure to identify risk factors, improper treatment planning, suboptimal surgical or prosthetic execution, and/or improper maintenance care. We can’t ignore the reality that patients could be suffering from peri-implant mucositis or peri-implantitis and should continually work towards understanding the disease, treatment and contributing risk factors.”
Are dental implants a panacea or should we strive to save teeth?
A recent article published in the January issue of The Journal of Dental Research, by noted clinicians W.V. Giannobile and N.P. Lang, addressed this important decision for and by the patient.
Dental implants have become an important treatment for the replacement of teeth lost due to disease, injury, or congenital tooth agenesis. Over the past 30 years the incorporation of dental implants into everyday clinical dental practice resulted in major improvements in the oral health of our patients, through enhancements in function, esthetics, and phonetics. Having been clinically trained in the Branemark Clinic in Gothenburg Sweden in the 80s, with the Branemark System of Hybrid Nobelpharma Implant restorations and continue to surgically place implants; I can attest to their great success. However, adverse outcomes associated with implants have come to the forefront of discussion groups in periodontology, oral surgery, prosthodontics, and implant dentistry relating not only to prosthetic (technical) failure but also persistent infections surrounding implants.
A trend affecting clinical practice over the past 2 decades has been the reduced emphasis to “save compromised teeth.” In fact, studies demonstrated those with less training in periodontology and implant dentistry generally applied reduced efforts in addressing tooth retention (Lang-Hua et al. 2014). It is noted less trained individuals are often recommending tooth extraction versus retention. As such, many teeth are being condemned at early stages given the expediency that lends itself to quickly rid a problematic tooth and provide a new tooth replacement implant. It is not unusual for many practitioners to recommend tooth extraction with modest tooth-associated ailments such as caries, need for endodontic therapy, or periodontal involvement. There are many scenarios where patients are advised to get rid of the compromised tooth and get the “newer, better” implant. It has recently been advocated that practice patterns should change to retain more teeth given the excellent long-term research proven track record of successful therapy for tooth preservation.
The erroneous belief of implants yielding a better long-term prognosis has now clearly been rejected in several comparative studies and systematic reviews. Teeth even compromised because of periodontal disease or endodontic problems may have a longevity that surpass by far, that of the average implant. We have been trained to preserve your teeth for your lifetime!
How effective is laser treatment for gum disease?
Nearly half of US adults have some level of Periodontitis, CDC study reveals: 47% of US adults aged over 30 years old and 70% of US adults aged 65 or older. (US Centers for Disease Control and Prevention) Information from American Academy of Periodontology.
Limited research suggests that the use of lasers as an adjunct to scaling and root planning (SRP) may improve the effectiveness of this procedure. SRP is a non-surgical therapy used to treat periodontal diseases. In addition, when the lasers are used properly during periodontal therapy there can be less bleeding, swelling and discomfort to the patient during surgery.
Can the use of lasers in periodontal therapy harm patients?
Yes and no. Each laser has different wavelengths and power levels that can be used safely during different periodontal procedures. However, damage to periodontal tissues can result if an inappropriate wavelength and/or power level is used during a periodontal procedure.
Does the research on lasers support their use in periodontics at this time?
At this time, there is insufficient evidence to suggest that any specific laser wavelength is superior to the traditional treatment methods of the common periodontal diseases, such as periodontitis.
Can I trust the claims in an ad for periodontal therapy performed with a laser?
It is important to beware of advertising that sounds too good to be true because it very well may be. A dental professional can help you separate fact from hype.
Will my insurance carrier cover the use of a laser in periodontal therapy?
Insurance carriers reimburse for the procedure being performed rather than the device used to perform it. Therefore, whether your periodontist uses traditional tools for treatment or lasers, your reimbursement will be the same for that specific procedure. Before having surgery, always consult with your insurance carrier to determine what procedures are covered in their plan. Dr. Bleier Comments, “As Lasers have such limited therapeutic use in gum disease treatments, I cannot justify charging for their use.”
Do you really need to have all your teeth extracted?
“You need to have all your teeth taken out”, may be one of the most devastating statements that a dentist can make. The thought that even one tooth needs extraction is a life changer for some. The consequences for that decision may be dentures or dental implants, but whatever the treatment, it is bound to change your lifestyle or make a dent in your pocketbook. But let me tell you, as a periodontist, as one who is responsible for determining ‘predictability’ or prognosis of your dental treatment plan, there are some people who are told that they need their teeth extracted that may be able to save their teeth.
Sometimes, a dentist or hygienist makes assumptions about periodontal disease that seem logical to him or her but may not be correct. There are countless examples in my practice of patients who were told to have their teeth removed because of periodontal disease who still have their teeth today. Of course, I have always held that most teeth can be saved in health and found it to be true for over 30 plus years of periodontal practice. Based upon the skills and experiences of periodontists themselves, they may not agree.
Now you would think that all treatment plans are the same, that if one dentist comes to a conclusion, that must be the conclusion. But you also know that there is the magic of the second opinion. The second opinion, whether in dentistry or medicine, sometimes finds a way that wasn’t considered by the person making the first opinion. Let’s give an example. A patient presents with a chief complaint of bad breath, some teeth that are loosening, tooth roots that are cold or hot sensitive, and many deep periodontal pockets. The patient is told that the disease is so severe that the teeth need to come out. We test the bacteria and find that the bacteria on the roots of the teeth are so aggressive that they are resulting in an exaggerated amount of bone loss for the teeth. We prescribe an antibiotic and within days, the bad breath is gone, and the teeth start to tighten. We then treat the disease by cleaning the roots of the teeth, treat the hot and cold root sensitivity and the teeth do better. They continue to tighten up. In a matter of months, the teeth are back to normal again.
If you are told that you have periodontal disease that will result in the extraction of teeth, the first thing that you should do is to get a second opinion with the right periodontist. The right periodontist has diagnostic and treatment tools that will help you reverse the disease in many cases. And if not, the right periodontist is the final judge on tooth longevity. You’ll have peace of mind knowing that you saw a specialist before making a life-changing decision.
How does your perio care fare?
Black triangles: prevalence and patient attitudes
One third of adults have unaesthetic black triangles, which are more appropriately referred to as open gingival embrasures. Besides being unsightly and prematurely aging the smile, black triangles are prone to accumulate food debris and excessive plaque. A recent study of patient attitudes found patient dissatisfaction with black triangles to rank quite highly among aesthetic defects which is mostly related to gum recession and bone loss from periodontal diseases. If you go online and search simply for “dental black triangles” you will be able to view hundreds of patients’ black triangle questions.
Better yet, call and schedule an appointment to learn your treatment options and how to help prevent this problem in the first place.
If your gums are receding and showing the roots of your teeth, you are losing the bone support underneath. The good news is that the gum recession and bone loss can be stgopped with proper treatment by a periodontist.
Periodontal procedures are available to stop further dental problems and gum recession, and/or to improve the esthetics of your gum line. This may involve working with other dentists as a team for your best treatment options.
Exposed tooth roots are dampering your smile and exposing the roots of teeth make your teeth appear too long. You may not be bothered by the appearance of these root exposed areas, but you cringe because of the exposed roots that are sensitive to hot or cold foods, sweets and other liquids.
These tooth roots sometimes decay. There are simple surface sealants available that can successfully eliminate this root sensitivity but this root sensitivity also can be a warning sign of early root surface decay.
Soft tissue grafts can be used to cover roots or develop new gum tissue which is absent due to excessive gingival recession. This can be done for one tooth or several teeth to even your gum line and reduce tooth sensitivity for a beautiful cosmetic result. A soft tissue graft, when needed, can reduce further recession and bone loss, next to dental tooth crowns, veneers and sealants.
Dr. Bleier received his Dental Degree (D.M.D.) from the University of Pennsylvania School of Dental Medicine, and his specialty training with a Clinical Certificate in Periodontology and a Clinical Fellowship in Periodontology while at Harvard School of Dental Medicine and a Certificate in Periodontology from the Veterans Administration in Boston, Massachusetts.
A beautiful new smile and improved periodontal health are your keys to smiling, eating and speaking with the comfort of your own natural teeth with confidence. Remember, dentistry offers good substitutes in many situations, but there is no excellent substitute for your own natural teeth.
How much will the treatment cost?
The cost of the periodontal treatment will vary depending upon your needs. After the periodontist has examined you and determined the appropriate treatment, he or she can provide you with an estimate of the cost. As you consider this health investment, keep in mind that treating gum disease is less costly – and better for your health – than replacing teeth lost to untreated gum disease.